April 2026 Newsletter
Welcome to our latest newsletter!
We’re diving into something a bit different: the world of science behind medicine and research, or shall I say, how science and medicine are researched and produce results and innovation. In this age of endless social media scrolls, of which I’m very guilty, many horse owners are bombarded with confusing claims, from miracle cures to anti-vax rants. It’s easy to get swept up in the hype, but we’re here to ground you in the facts. Science and data are your best ally against pseudoscience, and have driven to some significant advancements in equine care over the past two decades.


Let’s start with this: you’re wasting time and scrolling through your feed, and there’s a post claiming an herbal supplement can “cure” your horse’s laminitis overnight, or ulcers, no vet needed. Or maybe you are getting some rather odd, non-veterinary size related claims that pop up occasionally on Facebook. Sounds too good to be true? That’s because it probably is. In today’s digital Wild West, scams abound, anti-vax myths, anti-drug paranoia, and outright pseudoscience. These aren’t just harmless opinions; they can endanger your horse’s life and weaken your wallet. Understanding the scientific process empowers you to spot the real deal from the snake oil.
Misleading claims are in fact worse than wrong claims: when something is wrong, we just ignore and steer away, whilst when something is misleading, you end up wasting money, time and health/welfare before realising you are on the wrong path.
Let’s start by saying that science is not democratic: the speed of light is not decided by popular vote but by strict analysis, experimentation and observation. Things in science are or aren’t so it’s your choice to decide who to listen to, established sources or a random fella broadcasting from the parents’ toolshed. Reading, studying, and “knowledging” is time consuming and energy demanding but our success in life depends on the information we have available and the use we make of them.
Put it this way: if a treatment worked 100% of times with a 100% success, we would all be using that. This seldom happens in medicine, therefore we keep on studying and improving things, to get as close as possible to the 100%-100% scenario.
At its core, the scientific process is like a reliable trail ride: methodical, evidence-based, and always open to course corrections. It has historically been hindered by ignorance and indoctrination, such as the Holy Inquisition did to Galileo and Giordano Bruno, and has taken a while for us to have established research pathways.

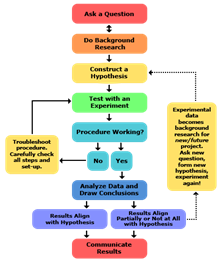
It starts with observation (a key word in science) and a question, for instance: “Does this new drug clear ulcers better than the ones we already have?” Then comes research, starting by digging into existing knowledge. Next, a hypothesis, a testable prediction, is formed. Experiments are designed to poke and prod that idea, collecting data rigorously. Horses are then treated with the new medication, examined, monitored, tested, and so on. If the results support the hypothesis, great!
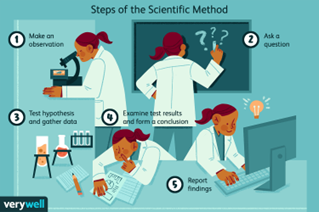
If not, back to the drawing board. Finally, findings are shared, interpreted, statistically analysed and peer-reviewed (which means examined, criticised and worked on by other experts in the same field), and built upon. It’s not about proving absolutes; it’s about building the strongest evidence possible.
And if the hypothesis revealed itself not to be true, the results are equally informative: like Edison said, “I have not failed, but found 1000 ways to not make a light bulb”.
This process is what underpins every treatment we recommend at our practice, and I’d like to think and hope in all vet practices. Unlike viral memes or celebrity endorsements, science demands reproducibility and scrutiny. Reproducibility is key in research and science: the same results must be obtained by the same tests and methods.
Take placebo-controlled studies, for instance. These are the gold standard for testing treatments. One group gets the real deal (like a new anti-inflammatory drug), while another gets a harmless placebo (a fake version – in most cases, plain water). If the real treatment outperforms the placebo, we know it’s not just wishful thinking. This weeds out the “placebo effect,” where improvement happens simply because we believe it will.
Then there are blind studies, which add another layer of honesty. In a single-blind trial, the horse owner (or researcher) doesn’t know who’s getting what, preventing bias from creeping in. Double-blind amps it up: neither the vet administering nor the owner knows, ensuring pure, unbiased results. These methods aren’t perfect, but they’re designed to minimize human error and hype.
In my personal (and admittedly humble) opinion, some of the most valuable scientific studies are the ones that end up concluding: “Don’t do that — we tried and it doesn’t work.” Let me explain. We all love being proven right. Our egos — especially in fields like medicine or vet med — crave confirmation that our favorite treatment, technique, or approach is effective. But the truly useful papers are often the ones that rigorously test a promising new intervention… only to show it makes no real difference (or sometimes even does harm). Those “negative” results are gold: they save time, money, and patients/animals from pointless or ineffective interventions. Knowing what doesn’t work is just as important as knowing what does, maybe even more so when it stops us from wasting effort on things that sound great in theory but flop in reality.
Sometimes it is however really hard if not impossible to design a study that proves efficacy of a specific treatment. An example for this would be proving with 95% confidence level that PRP, or stem cells, are better than leaving a tendon injury alone to heal. Designing such a study would involve having a population of let’s say 50 horses, roughly similar in size and age, sharing the same risk factors, in which we need to surgically produce the same exact tendon lesion (this is already impossible due to animal welfare rightfully). Then split the 50 into 2 groups, 25 get stem cells and 25 get an injection of water in the lesion.
Then all 50 horses must have the exact rehab program to avoid any possible discordance of variables. And all to be scanned at the same time. And ideally all should then have a sample of tendon collected after these have healed (in vivo or post mortem) to get it analysed under the microscope.
As you can imagine this is virtually impossible to do therefore, we tend to rely on a sentence of which I am also guilty myself: “in my experience”. This is a sentence that’s often used by all of us to back some of our ideas and past results. “In my experience, tendons do better after a PRP treatment compared to time and rest alone”. However, from a general point of view, “my experience” is one of the 8 billion experiences lived daily by all people on earth, so it does not carry any real scientific value, even if I’m pretty handy with the scanner. In medicine, we should always prefer something that’s tested, trialed and proved to be working (evidence based), rather than being anecdotally effective. But sometimes limitations of all sorts guide us to take pragmatic decisions. A further example of this? Tendon firing! You all have had a horse that “did well after tendon firing, in your experience”!!! But are you really sure about it? What are you comparing it to?
Building on individual studies, enter meta-analyses – the big-picture reviewers. Think of them as a roundup of all relevant research on a topic, like compiling dozens of trials on equine joint supplements. By pooling data from thousands of horses, meta-analyses spot patterns that single studies might miss, giving us rock-solid conclusions.

For example, a meta-analysis might confirm that certain vaccines reduce infection rates by 80%, backed by stats from across the globe. It’s this cumulative wisdom that guides our advice.
Do you want a good example of meta-analysis? A 2015 comprehensive assessment by the Australian National Health and Medical Research Council reviewed over 1,800 studies and concluded that homeopathy is not effective for treating any health condition, performing no better than a placebo. It found no reliable evidence that homeopathy works for 68 different illnesses, leading to international recommendations against its use. Music to my ears
Acupuncture? Same gig, studies debunk acupuncture by showing it is no more effective than sham (placebo) acupuncture, suggesting pain relief is due to the patient’s expectation or the ritual of care rather than specific meridian points. Research indicates that placing needles randomly or not piercing the skin works just as well as traditional, targeted acupuncture.
Sadly, nowadays social media amplifies the opposite: pseudoscience that cherry-picks data or ignores the process altogether. Anti-vaxxers claim vaccines cause more harm than good, ignoring mountains of placebo-controlled, double-blind evidence showing they’re safe and effective. Anti-drug crusaders push “natural” alternatives without any testing, risking untreated infections or colic. These scams prey on your good will, promising quick fixes while dismissing science as money grabbing conspiracies. Not long ago in Italy we had a 6 years old kid dying of an ear infection, as the parents rather listen to an omeopathic person for something that could have been treated with routine antibiotics, that’s criminal to me.
I remember having an argument with a classmate of mine in uni, as she became a fierce anti-vaxxer during covid, only to find out that she was still going out vaccinating animals at £60 a pop. Nevertheless, recently some idiots are also suggesting that vaccinating animals is bad for them. This is something I don’t want to elaborate here too much or I’m going to lose the plot however I understand that current rules of racing are making equine vaccinations a palaver (coupled with online certification and app signature) BUT money spent on vaccines are really the most cost effective: vaccinating a horse for herpes costs a fraction of what it costs to treat a group of horses suffering from EHV infection.

Recently I had a real fun conversation/argument with an owner of a horse with an infected leg, which can be summarised as the below two lines:

Customer: No, I’m not giving the horse antibiotics because they’re bad for him.
You: Lady, what’s worse for the horse is dying.
You can imagine how frustrating it is to hear such random stuff after nearly 20 years of treating fat legs and doing half a decent job at it.
Ivermectin has recently become a wonder treatment, from worms to cancer passing through hemorrhoids, voiced by the likes of Joe Rogan, @LittleStrawberry21 and @Banana69 on YouTube, well known worldwide in the fields of experimental medicine, pharmacology and data analysis. For once I totally agree with them, I think you guys should all start eating Ivermectin, we sell it at a real affordable price and we got plenty in stock, natural selection will do the rest.
In today’s rapidly evolving world of medical innovation, pseudoscience and misinformation are increasingly undermining public confidence in proven scientific breakthroughs. False claims about vaccines, gene therapies, and emerging cancer treatments have created confusion and fostered distrust in global health initiatives.

During the COVID-19 pandemic, for instance, 5G skeptics went so far as to blame wireless networks for the spread of the virus—illustrating how easily fear can eclipse facts. These unfounded beliefs spread swiftly through social media, often drowning out the voices of experts and researchers. When pseudoscience seeps into government decision-making, the impact becomes even more damaging: poor policy choices emerge, research funding is misdirected, and long-term health strategies lose focus and credibility.
In the short term, we will face preventable health crises; over time, innovation slows and public trust erodes. mRNA research and precision medicine, for example, hold extraordinary potential to prevent and treat diseases more effectively. Yet, when misinformation takes root, it hinders cooperation and public acceptance. Rebuilding trust demands open communication, accessible education, and consistent reliance on evidence-based science.
Where has all of the above maxi explanations led us? Well, over the last 20 years, equine veterinary medicine has leaped forward, transforming how we care for all domestic animals. Issues that were hard to resolve when I graduated, are now routinely treated and diagnosed.
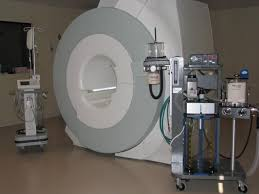
Standing MRI and low-field MRI systems now enable detailed imaging of the foot, fetlock, and hock without general anesthesia, pinpointing subtle lameness issues like navicular disease or stress fractures early. The first MRI I had seen was in Hagyards in Kentucky in 2008, it was something mythological to witness, a 1.5 tesla magnet, 1million dollar worth of kit, nowadays these can be rented together with a container! Advancements in portable CT scanners provide 3D views of complex fractures and soft tissue, which has enhanced the way we repair and understand fractures. Advanced endoscopy, including dynamic scopes on the gallops, has become more and more available and affordable.

Echocardiography with Doppler and holter monitoring and event recorders track intermittent arrhythmias over 24-48 hours, essential for endurance horses. 3D echocardiography assesses myocardial function in myocarditis cases linked to viral infections. Cardiology has leaped forward massively, allowing us to understand more and more about horse performance and issues.
First opinion equine veterinary work, which forms the core of everyday care for most horses and vet practices, including obvs ourselves, can now integrate these advancements into routine yard visits. We all have lots more expensive toys in the car compared to when I graduated. Portable ultrasound, digital radiography, and stall-side blood analysers have become standard, enabling faster diagnoses and treatments without specialist referrals. Wearable tech like smart heart monitors and trackers allow us to calculate vital signs proactively, while telemedicine consults link field vets to experts for real-time advice on everything from wound management to vaccination protocols. This shift empowers first opinion vets to handle 80% of cases on-site, in our case probably even more close to 95%, reducing stress for horses and owners while bridging the gap to advanced care when needed.
In terms of repro medicine, we are now playing god as we are able to clone animals. Intracytoplasmic sperm injection (ICSI) has completely changed the way we breed sport horses, allowing fertilization of oocytes from subfertile mares using a single sperm—success rates now exceed 30% for foal production in elite programs. Frozen embryo transfer (ET) and oocyte cryopreservation enable year-round breeding schedules, preserving genetics from aging performance mares. Hormonal protocols with deslorelin implants and ultrasound-guided ovulations improve twin reduction and synchronization for commercial studs.

Veterinary and Human medicine and more and more interconnected and run together in allowing maximal success treatment without long term issues that could hinder treatment efficacy. I’m obviously referring to antibiotic resistance, which has become a hot topic and is a key factor in us deciding what antibiotic to use, or even what we have available. A multidisciplinary approach is a must nowadays as our understanding of the world keeps on broadening and expanding. You might have heard of H5N1 bird flu, and how that’s so dangerous as could mutate to being able to affect people and not only birds. Behind all of this knowledge and research there is a team of Gov’t vets collaborating with specialist virologists, sampling, testing, researching.

Altogether, such cross-disciplinary innovations, crossing the boundaries between human and veterinary medicine, have slashed recovery times, boosted foaling rates, cut lameness recurrence, improved surgical techniques, provided us with more advanced and specific treatments, fueling a healthier global equine population.
Looking ahead, the future is bright—and tech-savvy. I’m pretty old school and still trust my hands and eyes more than most of tools available, but it would be silly not to accept these ever-progressing changes. Expect wearable devices tracking your horse’s vitals in real-time, AI-driven diagnostics for faster, more accurate calls, and telemedicine for remote consults.

Stay healthy and steer away from bull$hit, I hope you enjoyed reading me ranting about a lot of different stuff in this newsletter!
Fair play if you’ve made it this far!
All the best,
Paolo
